Colorectal Surgery
Colorectal Surgery by Dr. Iraniha
Each year, more than 600,000 surgical procedures are performed in the United States to treat a number of colon diseases. Diseases of the colon and rectum that might requiring surgical intervention include diverticulitis, ulcerative colitis, Crohn's colitis, colonic polyps not amenable to removal by colonoscopy, tumors (benign and malignant), hemorrhage, as well as other entities.
Patients undergoing colon surgery often face a long and difficult recovery because the traditional "open" procedures are highly invasive. Most open surgeries of the colon require long incisions, and surgery results in an average hospital stay of 5-8 days and usually requires 6 weeks for recovery.
Since 1990, virtually all types of colorectal procedures are accomplished using minimally invasive techniques. These laparoscopic techniques replicate exactly the operation undertaken through large abdominal incisions. The laparoscopic colorectal operations offer many of the same advantages to patients as do other laparoscopic operations. Patients tend to experience less pain, fewer wound complications, a shorter length of hospital stay, faster return of bowel activity and a quicker return to normal activity.
Laparoscopic colon surgery is a new technique that is rapidly gaining popularity. The surgeon makes about four or five small incisions. A laparoscope is inserted into one of the openings, allowing the surgeon to see inside the abdomen. Instruments are inserted through the other openings and are used to remove the diseased section of bowel and reattach the healthy segments ('end-to-end anastomosis'). A slightly larger incision is usually made to remove the diseased section of colon from the body. The surgery takes 2 to 3 hours. Depending on the type of procedure, patients may leave the hospital in a few days and return to normal activities more quickly than patients recovering from open surgery.
Before & After Laparoscopic Colorectal Surgery
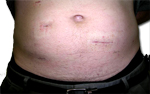
Left Colon Resection
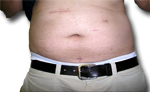
Right Colon Resection
Laparoscopic techniques have been applied to virtually all types of colorectal procedures. The diseases most commonly treated with laparoscopic operations include complications of diverticular disease, Sigmoid volvulus , and benign colorectal neoplasms. Closure of colostomies after a Hartmann's procedure or the creation of a colostomy can be easily accomplished laparoscopically . Treatment of colorectal malignancies with laparoscopic resections is also very well established. It has been shown that adequate en bloc resection and regional lymph node dissection are feasible and safe using the laparoscopic technique. Quantitative measures of the size of the specimen, the length of the mesentery, and the number of lymph nodes present suggest that the quality of the operation for colorectal malignancies is maintained when it is performed laparoscopically. The rate of intraabdominal complications such as anastomotic leaks and intraabdominal abscesses are not different from that observed with open operations. This is not surprising, since the extent of dissection and the magnitude of resection are the same for both techniques. Moreover, identical techniques are used for the construction of anastomoses.
One of the most common diseases that require laparoscopic colectomy is diverticulitis. Mild cases of diverticulitis can be treated with changes in diet, rest and antibiotics. But recurring diverticulitis and more serious cases may require surgery to remove the diseased portion of the colon.
Diverticula are small, bulging pouches that develop in the wall of the large intestine (colon). Usually they are most numerous in the sigmoid colon. Many people develop diverticula (a condition called diverticulosis), especially after age 50, and in most individuals they cause no problem. However when diverticula become infected or inflamed (a condition called diverticulitis), they can cause pain, fever and nausea. Diverticulitis ranges from mild pain to life-threatening infection. In rare cases, a pouch can rupture, spilling intestinal waste into your abdomen. This is a medical emergency requiring immediate surgical intervention.
Only 15 to 20 percent of people who have diverticulosis develop diverticulitis. The major factors associated with diverticulitis include advancing age and lack of dietary fiber. In many cases people can help prevent this disease simply by including more high-fiber foods in their diet.
Diverticulitis is common in industrialized nations such as the United States, where the average diet is high in refined carbohydrates and low in fiber. Too little fiber contributes to small, hard stools that cause increased pressure in the colon.
Diverticulitis can feel like appendicitis, except the pain will be felt in the lower left side of the abdomen, instead of the lower right. The pain can be severe and come on suddenly, or it can be mild and fluctuate in intensity.
Treatment of diverticulitis depends on the severity of symptoms and how many acute episodes the patient has experienced. If symptoms are mild, a liquid or low-fiber diet and antibiotics may be recommended. Those at risk of complications, or who experience recurrent attacks of diverticulitis, may require surgery to remove the diseased portion of the colon.
The patient's age at the time of the attack may be an important factor in the treatment plan. It is recommended that patients younger than 50 receive more aggressive treatment than patients older than 50. Studies have shown that younger patients may be at a higher risk for recurrent attacks and complications such as a perforatation and abscess formation.
About half of those who have diverticulitis require hospitalization and many need intravenous antibiotics. In serious cases of diverticulitis surgical resection of diseased bowel is indicated. Depending upon the patient's condition, laparoscopic methods may be used in place of traditional surgery. Laparoscopic procedures usually require smaller incisions and enable a faster recovery for the patient. If colon becomes so inflamed that it is not safe to rejoin the colon and rectum or the patient experiences a life-threatening infection like perforated colon with peritonitis then surgeon will perform a colostomy. The colostomy is usually temporary until the infection and inflammation clear. To create a colostomy, the surgeon makes an opening in the abdominal wall. The colon is then brought out through the opening, and waste passes through the opening into a bag. Once the inflammation has healed, perhaps several months later, the surgeon may be able to perform a second operation to reconnect the colon and rectum.
Even though the laparoscopic colon surgery was introduced approximately 15 years ago, yet, only 3% of all colon resections are performed this way in the United States. The laparoscopic colon surgery is an advanced procedure that takes a long period of time to master. At Newport Laparoscopy, Dr. Iraniha has substantial experience in advanced laparoscopic colorectal surgery and offers this minimally invasive procedure for a variety of colorectal diseases, including colon cancer.
More recently, colorectal minimally invasive surgery can be performed using robotic technology. The da Vinci System is a robotic surgical platform designed to enable complex procedures of all types to be performed. There have been some major benefits experienced by surgeons using the da Vinci Robotic Surgical System over traditional laparoscopic approaches. These benefits are greater surgical precision, increased range of motion, improved dexterity, enhanced visualization and improved access.
At NEWPORT LAPAROSCOPY, Dr. Iraniha performs robotic colorectal surgical procedures. After a thorough evaluation, Dr. Iraniha will determine whether robotic colorectal surgery is appropriate for a particular patient's situation.
Do you neeed to set an appointment with Dr. Iraniha?
Click on the Contact Us button to start the appointment process. Thank you!
