Anti-Reflux Procedures
Anti-Reflux Procedures by Dr. Iraniha
Gastroesophageal reflux disease (GERD), also known as acid reflux, is a 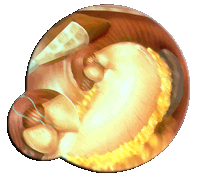 condition in which stomach acids or bile salts back up into the esophagus producing a burning sensation behind the breastbone and esophageal irritation or inflammation. Normally, acid is trapped in the stomach by a circular band of muscle called the lower esophageal sphincter (LES), which remains closed except when swallowing. If the sphincter relaxes abnormally or becomes weakened, stomach acid tends to back up, causing symptoms of heartburn. This can also be exacerbated by the presence of a hiatal hernia (when part of the stomach is protruding through the diaphragm and into the chest).
condition in which stomach acids or bile salts back up into the esophagus producing a burning sensation behind the breastbone and esophageal irritation or inflammation. Normally, acid is trapped in the stomach by a circular band of muscle called the lower esophageal sphincter (LES), which remains closed except when swallowing. If the sphincter relaxes abnormally or becomes weakened, stomach acid tends to back up, causing symptoms of heartburn. This can also be exacerbated by the presence of a hiatal hernia (when part of the stomach is protruding through the diaphragm and into the chest).
An estimated 17 million Americans currently suffer from heartburn and other symptoms of GERD. For many people, it can be treated with the correct combination of lifestyle changes and medication. For others, surgical intervention can help to eliminate the symptoms and prevent further damage to the esophagus.
The main symptoms of GERD can be divided into typical and atypical symptoms. Typical symptoms include a burning sensation in the chest, and regurgitation of food. These symptoms are general, and not necessarily specific for reflux disease. For instance, patients may experience chest pain or burning as a result of a primary cardiac problem, or they may be a manifestation of another primary esophageal disorder. It is imperative that the cause of the symptoms be clearly delineated by your physician so the proper therapy may be instituted. Regurgitation is also a relatively common complaint.
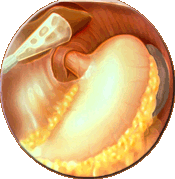 Atypical symptoms of GERD include asthma, chronic sinusitis, chronic hoarseness, difficulty swallowing (dysphagia), vomiting, choking sensation at night time, pneumonia, and excessive salivation, sore throat, coughing, wheezing. Certain medical conditions, foods and medications may also exacerbate GERD by their ability to lower the resting pressure of the LES. Sometimes GERD can cause serious complications. Inflammation of the esophagus from stomach acid causes bleeding or ulcers. In addition, scars from tissue damage can narrow the esophagus and make swallowing difficult. Some people develop Barrett's esophagus, where cells in the esophageal lining take on an abnormal shape and color, which over time can lead to cancer.
Atypical symptoms of GERD include asthma, chronic sinusitis, chronic hoarseness, difficulty swallowing (dysphagia), vomiting, choking sensation at night time, pneumonia, and excessive salivation, sore throat, coughing, wheezing. Certain medical conditions, foods and medications may also exacerbate GERD by their ability to lower the resting pressure of the LES. Sometimes GERD can cause serious complications. Inflammation of the esophagus from stomach acid causes bleeding or ulcers. In addition, scars from tissue damage can narrow the esophagus and make swallowing difficult. Some people develop Barrett's esophagus, where cells in the esophageal lining take on an abnormal shape and color, which over time can lead to cancer.
If more serious symptoms (such as severe heartburn, difficulty swallowing or weight loss) are present or if heartburn is not relieved by medications, then further testing is required including upper endoscopy, barium swallow, cardiac evaluation, esophageal manometery and esophageal pH study
What involve treatment for GERD?
Treatment for GERD may involve one or more of the following lifestyle changes, medications, or surgery. The goals of therapy for GERD include: a) Symptomatic relief; b) Resolution of esophagitis (inflammatory changes of the esophagus as a result of abnormal acid exposure); and c) Prevention of complications.
The first step in treating GERD includes lifestyle and diet modifications which include elevation of the head of the bed, limiting or avoiding foods that can exacerbate GERD, such as alcohol intake, quite smoking, losing weight, and not lying down for several hours after eating.
The second step in treating GERD includes medications such as antiacids, H2 blockers, proton pump inhibitors (PPI) and prokinetic medications,
Patients are considered for surgical therapy of GERD if:
1. Medical therapy fails to control their symptoms despite large doses of PPI, or prevent complications of GERD such as Barret's esophagus (thought to be a precancerous lesion), esophageal stricture (leading to obstruction and inability to eat), ulcer formation, and bleeding.
2. Atypical symptoms persist (asthma, sinusitis, cough, hoarseness, etc...)
3. A patient cannot take mediation because of undesirable side effects, poor compliance, or unwilling or unable to pay for long-term medical treatment.
4. A patient prefers surgery rather than life long medical therapy.
The purpose of surgery is to repair the stomach valve that is allowing acid to leak into the esophagus. Certain tests will be performed prior to surgery to ensure that the patient's condition is likely to be helped by surgery. Patients are generally evaluated using endoscopy, 24-hour pH studies, manometry or barium X-rays.
The most common anti-reflux surgical procedure performed for treatment of GERD is a Nissen fundoplication . The upper portion of the stomach (the fundus) is wrapped around the lower portion of the esophagus and anchored securely below the diaphragm. If there is a hiatal hernia, the hernia will also be fixed.
The operation is effective long term in stopping esophageal reflux and relieving symptoms. More than 90 percent of patients who have fundoplication surgery are able to leave hospital the next day, eating a soft diet. Most people are able to return to their normal activities, work or school within one to two weeks after surgery. The satisfaction rate with this procedure is 96 percent at one year.
Fundoplication has undergone several improvements. Using a laparoscope and five small incisions, the surgeon can operate without making a large incision to open the abdomen. The operation is the same, but the patient is spared the long hospital stay and prolonged recovery time of open surgery. There is also less pain after surgery, less chance of wound infection and smaller scars because of the smaller incisions.
Surgical complications occur in 2 to 4 percent of patients who undergo laparoscopic surgery. The risk of death after this operation is less than one in 500.
After surgery, there may be a delay in intestinal recovery that causes bloating, gagging, and vomiting, which resolves in a few weeks. If symptoms persist or if they start weeks or months after surgery, particularly if vomiting is present, then surgical complications are likely. Complications are uncommon, but include and not limited to bleeding, infection, damage to the internal organs such as esophagus, spleen, bowel, major vessels, nerve, numbness, requirement for re-operation, transfusion, post op pulmonary emboli, deep venous thrombsis, pneumonia, hear attack, stroke, bowel obstruction, and incisional hernia. If the fundus is wrapped too tightly, patients may have difficulty swallowing or be unable to burp. In rare cases following surgery, muscles spasms after swallowing food can cause intense pain, and patients may require a liquid diet, sometimes for weeks. The surgery may need to be repeated under certain circumstances: if the wrap has slipped or is too loose; or if the patient has persistent difficulty in swallowing, hernia, or recurrent ulcers. Even with repeat surgery, results are excellent.
Do you neeed to set an appointment with Dr. Iraniha?
Click on the Contact Us button to start the appointment process. Thank you!
